Dialysis treatments, hemodialysis, peritoneal dialysis, and continuous renal replacement therapies filter out salt, water, and waste from your blood. The treatments replace lost kidney function and can be temporary or ongoing. Your urologist creates dialysis access that allows blood to be drawn, filtered, and circulated back to your body. Here are the steps of dialysis treatment:
Hemodialysis Treatment Steps
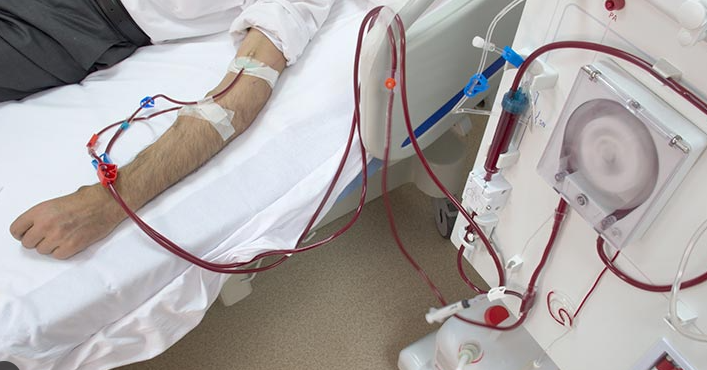
Your urologist can recommend hemodialysis treatment, which involves filtering your blood through an external machine. The steps include creating a dialysis access weeks before the first treatment. Dialysis or vascular access can be a fistula that connects an artery to a vein using your own tissue. Urologists may also use grafts, which are tubes made of synthetic material. A catheter is also used to place a temporary solution in a large vein in your neck or chest. On the day of your first dialysis, the doctor measures your weight, temperature, and blood pressure to monitor fluid levels. Needles connected to the filtration machine are then inserted into the fistula or graft to begin drawing blood.
One needle draws blood from your body into the machine, and another returns the filtered blood to the body. Inside the machine, blood passes through a dialyzer filter that removes waste and excess fluid. The machine can also feature a dialysis solution that removes toxins through diffusion. Nurses monitor your vitals and machine settings throughout the process. Once the session is completed, the needles are removed, and pressure is applied to the vascular access to prevent bleeding. Your doctor can measure your weight and pressure once more and recommend a few minutes of rest before you’re released. The procedure is usually done at the hospital or home and involves sitting or lying on a couch or recliner bed.
Peritoneal Dialysis Steps
In other cases, your urologist might recommend continuous ambulatory peritoneal dialysis (CAPD) or automated peritoneal dialysis (APD). These two types of procedures are known as peritoneal dialysis. CAPD involves filtering your blood several times a day, while APD uses a machine to filter blood during the night as you sleep.
Peritoneal dialysis uses the peritoneal membrane in your abdomen to filter blood. Before treatment begins, a catheter is surgically placed into your abdominal cavity, where it remains for the dialysis session. Your urologist then fills one bag with a dialysis solution and connects it to a catheter. An empty bag that collects the waste is also attached to the catheter using tubes and clippings. Your urologist should provide a wheel stand you can use to hang the bags.
The dialysis solution is introduced to the peritoneal cavity through the catheter. Also known as dialysate, this solution absorbs waste and excess fluid from your blood through the peritoneal membrane. Filtration can take a few hours, after which the used solution is drained out through the catheter into the empty bag. A fresh dialysate is introduced to repeat the process. Follow your urologist’s instructions to keep the vascular and peritoneal access clean and safe, including sterilizing the catheter to prevent infections. After a few sessions with your urologist, you may be able to master the process to safely perform peritoneal dialysis on your own, which could give you more flexibility to resume daily activities.
Visit a Urologist to Create Your Dialysis Access Today
Kidney dialysis treatments involve creating access to allow the use of fistulas, grafts, and catheters. Experienced surgeons create the access a few weeks before your first dialysis. Contact a urologist today to find out more about dialysis access and treatment steps.